| Any advice given and opinions expressed in this article are those of the author and do not necessarily reflect the views of Chiesi Limited. All content in this article is for informational and educational purposes only. |
In this article, we’ll explore the concept of person-centred care and the strategies available to facilitate this collaborative approach. Respiratory Pharmacist and National Public Health Trainer, Darush Attar-Zadeh will also offer his thoughts, with examples of person-centred care in respiratory and ways to help deliver this care approach.
What is person-centred care?
Person-centred care is a healthcare approach that focuses on the care needs of the individual. In this model, the person receiving care is actively involved in decisions about their own health and well-being.1, Healthcare professionals (HCPs) aim to understand and respect patient’s preferences, needs, values and goals to guide clinical decisions.1,
Person-centred care ensures that people are always treated with dignity, compassion and respect.
A central approach to person-centred care is shared decision making (SDM). This is a process in which a healthcare professional works together with a patient to reach a decision about care – considering both evidence and the individual’s preferences, beliefs, and values.2, This approach ensures the patient is well-informed, understands the available options, and is actively engaged in the decision-making process.
SDM aligns with the person-centred care model, where the goal is to tailor healthcare to the individual, fostering a collaborative and respectful relationship between the person and their healthcare team.2,
The evidence suggests patients want to be involved in making decisions about their own healthcare.3, When people have the opportunity and support to make decisions about their care and treatment in partnership with health professionals they:2,
- are more satisfied with their care
- tend to choose less invasive and costly treatments
- are more likely to stick to treatment plans and medicine adherence
- are less likely to use emergency hospital services.
Not only do patients benefit from shared decision making being embedded as standard practice, but healthcare systems do too. As patient engagement increases, staff performance and morale see a corresponding increase.4,
There is evidence that the implementation of person-centred care models also contributes to better use of resources and decreased costs.2,
While person-centred care is generally considered a positive and beneficial approach, it is not without its limitations. There are challenges of:5,6,
- risk for compassion fatigue – where healthcare staff may feel overloaded by duties and engagement in their patients, experiencing feelings like hopelessness and anxiety and eventual lessening of compassion
- exclusion of certain groups
- unfairness due to empathy – where a patient may get more attention than others due to a HCP being ‘too empathetic’
- time and resource limitations
- health literacy.
When it comes to respiratory health and delivering person-centred care, the challenges may vary depending on the condition. Darush Attar-Zadeh, who has a keen interest in preventative medicine and is actively involved in training around behaviour change techniques, discusses some of the challenges in asthma and COPD from his perspective:
| Asthma | COPD |
| “In a 20-minute annual asthma review consultation with a patient living with asthma, it can be quite challenging to cover what’s needed around effective preventative medicine and offering time to the patient to ask questions and summarise key outputs. It’s important to ensure follow up consultations are completed (especially for patients who have a history of not being fully controlled), of which can also be delivered via groups, that we signpost to reputable sources and use aids to support learning.” | “In a 20-minute review with a patient living with COPD, it can be challenging to support a patient who has numerous uncertainties on what they can do to prevent and treat it. We must address any myths and perceptions of COPD as the term can mean different things to different people. It’s important to ensure modifiable risk factors are clear to the patient, including the damaging effects of inactivity, indoor and outdoor pollution including tobacco exposure, poor housing, not being vaccinated and not maximising the use of inhaled treatments. Health literacy and cultural beliefs should also be considered.” |
Person-centred care: a core NHS principle
The NHS has highlighted person-centred care as a core principle in the Long Term Plan, committing to giving people greater control over their own health.7, Respiratory conditions are one of the key areas of focus.7,
The NHS is on a journey to make personalised care ‘business as usual’ through a range of personalised care packages:8,9,
- rolling out the NHS Comprehensive Model for Personalised Care (which brings together six programmes aimed at supporting a whole population, person-centred approach), so that 2.5 million people can have choice and control over support for their mental and physical health within the next decade
- ensuring up to 200,000 people benefit from a personal health budget within the next five years, so they can control their own care, improve their life experiences and achieve better value for money
- deploying extra Social Prescribing Link Workers so more people are connected to wider community services for improved health and well-being – since 2019, more than 2.5 million people have been referred to Link Workers, and the numbers are rising fast.
Similarly, the National Institute for Health and Care Excellence (NICE) has also been working to help put SDM at the centre of the way care and treatment is given.
NICE was one of the first national health institutes globally to formally support SDM practice and research,10, publishing guidelines recommending SDM be part of everyday practice across all healthcare settings.11, The guideline offers advice on how to engage people in the SDM process through honest conversation and by providing resources before, during and after appointments. NICE also addresses SDM at a national level with Quality statement 4 in its clinical guideline covering the components of a good patient experience.
Person-centred care in practice
The implementation of person-centred care at a national level involves healthcare providers, policymakers, patients, and other stakeholders. It also requires services and practitioners to be open to a wide range of approaches and initiatives. Some of these are already being done, offering inspiration, support, and important success criteria, for those looking to put person-centred care into practice.
Some initiatives in place, or being explored, for helping to deliver person-centred care and SDM include:2,12,
| National Voices collaborative care and support planning | National Voices highlighted the four main steps of the care and support planning process, identifying a number of principles to help ensure the process is truly person-centred. These can be found in their interactive guide. |
| House of Care model | A model where HCPs and patients with long-term conditions come together as equal partners to discuss care and planning. It is often referred to as a ‘whole-system’ approach: all the elements need to be in place for change to happen. An example would be an Integrated Care Board (ICB) Clinical Reference Group for Respiratory – shaping local care. |
| Experience-based co-design | An evidence-based method that involves gathering experiences of patients, health and care professionals, bringing them together to develop service improvements. It helps frontline staff to re-frame their approach, see things from patients’ perspectives, and work to identify often small changes that make a big difference to patients’ experience of care. |
| Personal health budgets | A personal health budget uses NHS funding to create an individually agreed personalised care and support plan. They can be used to pay for a wide range of items and services, including therapies, personal care and equipment, allowing individuals to have more choice and control over the health services and care they receive. |
Bringing SDM into day-to-day patient interactions requires a specific approach from healthcare professionals, both at a practice and individual patient level.
At a practice level, this can include:2,13,
- training and education for all HCPs – focusing on effective communication, empathetic listening and SDM techniques
- use of decision aids – integrating decision aids such as informational brochures and interactive online tools to increase patient involvement, using resources such as the International Primary Care Respiratory Group (IPCRG) Asthma Right Care or COPD Right Care packs
- encouraging people to use question prompts – checklists or documents to spark ideas about questions to ask during interactions with health professionals
- feedback mechanisms – establishing ways of collecting feedback from patients to improve engagement.
At a patient level, this can include:13,,14,,15,
- giving patients access to their medical records – for example, through the NHS app or Patients Know Best (PKB), an online service for patients to securely access personal health records
- establishing rapport and sharing responsibility
- asking open-ended questions – to understand patient concerns, expectations, and preferences on available treatment options
- avoiding jargon.
“Developing greater awareness of different cultural beliefs is important to meet the diverse needs of all patients and families, so training around this should not be overlooked.” Darush says. “Elements of health literacy are also important and can present challenges in the way we provide care.” Recognising and respecting diverse cultural contexts can help with aligning treatment plans with patients’ values, potentially influencing health care outcomes.16,
In the view of health literacy, adapting communication strategies and tailoring information to patients’ comprehension levels can help to ensure patients understand and can make informed decisions about their own health.17, This could be adapting and simplifying language to decrease the risk of misunderstanding, providing examples that are relevant to the individual’s lifestyle and cultural context, using visual representations of data, and integrating decision aids into care.17,
Case studies: What does person-centred care in respiratory care look like?
Darush outlines what person-centred care can look like in respiratory care, covering inhaler device choice, smoking cessation and self-management*:
-
1. Inhaler choice - right patient, right device
A 21-year-old patient living with asthma attended an annual review via a video consultation (accuRx). He was quite happy with his current inhaler and I observed his technique with his dry powder inhaler (DPI), which was good. He prepared his device nicely, breathed out away from the device, formed a nice seal around the mouthpiece, tilted his chin up and then inhaled quickly and deeply, followed by a nice breath hold for around 10 seconds.
He also had a second device that was in a pressurised metered dose inhaler (pMDI) without a spacer (as he refused to have one after further investigation) and I observed he struggled to master the technique. After a discussion about what he knew about poor technique, and the unintended consequences, he agreed that it would be better to find an alternative device that was consistent with his DPI.
When I mentioned the device he was on was also licensed for Maintenance and Reliever Therapy (MART), he opted to go down that route and was pleasantly surprised that this option was available. He was also happy to see the dosing schedule clearly on his MART asthma plan, where he felt reassured he wouldn’t be exceeding the daily dose and when to seek help if symptoms deteriorated.
-
2. Smoking cessation
A 65-year-old smoker living with COPD attended the practice for an annual review and flu vaccine. He reported that he was struggling walking with his dog and visiting the supermarket, and found his general well-being was bothersome.
Very Brief Advice (VBA) was offered, which is a simple and powerful intervention designed to be used opportunistically in less than 30 seconds in a consultation. It involves three steps:18,
1. Ask: Do you smoke?
2. Advise: Did you know the best way to stop is with a combination of support and treatment, which is available on the NHS?19, You’re three times more likely to stop and it’s one of the best treatments we have available to help with your current symptoms. You’re also five times less likely to get flu and twice less likely to get pneumonia20,
3. Act: Would you like me to signpost you to one of the advisors we have in the practice?
The gentleman decided to stop smoking after seeing a trained advisor who could offer designated time to the patient. The session involved assessing motivation, picking a day to go smoke free (decided by the patient), exploring treatment options, checking their carbon monoxide (CO) readings, as well as exploring barriers and past quit attempts.
-
3. Pulmonary rehabilitation
A 72-year-old lady living with COPD walked into a community pharmacy with her daughter to get her COVID-19 vaccine. The pharmacist was quite surprised to see her as she hadn’t been out for quite a while. The lady mentioned that she is not as active as she used to be as she has to stop for breath after walking 5 minutes or so. Even getting dressed has become a challenge for her.
The pharmacist, who had completed recent training around the benefits of pulmonary rehabilitation (PR) and was conscious not to use words that may put her off (for example, exercise), offered VBA. The IPCRG offers a useful pulmonary rehabilitation referrer’s guide.
1. Ask: How has breathlessness changed your life? What troubles you most about being breathless?
2. Advise: Breathlessness whilst moving around is normal. It is not harmful or dangerous to feel short of breath whilst moving. PR helps you breathe better, feel good, do more and I strongly recommend it. Have a look at what other breathless people say about it.
3. Act: Patients I know have gone to this local service; the wait times have reduced dramatically. I can call your GP to arrange this if you like.
The lady decided to go after some more gentle persuasion from her daughter. Her daughter now says she feels less like a carer since the PR sessions and her mother is far more independent. The lady also mentioned it was a great opportunity for her to meet others with a similar experience, to learn to control her breathlessness and to reduce the impact of it on her life. She has even started singing.
*insights from personal clinical experience.
Watch Respiratory Nurse Consultant, Joanne King, explain the importance of ensuring patients are using the most suitable device.
Key takeaways
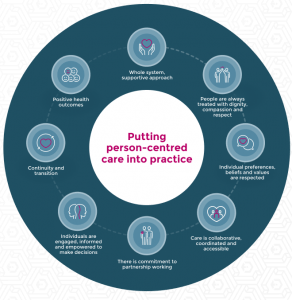
Graphic author’s own.
Encouraging people to become active participants in their health requires not only a combination of strategies, tools and activities but a mindset that values this collaborative healthcare method. It needs a whole system, supportive approach, integrating services including health, social care, public health and wider services around what’s important to the individual, as well as commitment from healthcare providers and patients.
The NHS roll out of the Comprehensive Model of Personalised Care and ambitions to make personalised care a priority in respiratory is an important takeaway – especially as it is now understood that hospital admissions for lung disease have risen over the past seven years at three times the rate of all admissions generally.21,
The principles and strategies outlined are all steps in the right direction, although Darush notes there could be obstacles in fully engaging shared decision making. “Workforce capacity, staff morale, patient waiting times and burnout are a few examples that may play a part in compromising the ability to perform shared decision making to its full extent.” The key lies in identifying potential gaps and actively working to fill them. Ultimately, every level of the health system has a role to play in creating the right conditions for person-centred care to flourish.
Visit our resource page to access useful information for you and your patients.








